 The Royal Osteoporosis Society and the APPG on Osteoporosis and Bone Health have published a new report exposing how a “postcode lottery” in NHS prescribing leaves over 1 million women without access to vital bone-strengthening treatments. This analysis calls for unified, system-wide policy reform to ensure equitable medication pathways for all.
The Royal Osteoporosis Society and the APPG on Osteoporosis and Bone Health have published a new report exposing how a “postcode lottery” in NHS prescribing leaves over 1 million women without access to vital bone-strengthening treatments. This analysis calls for unified, system-wide policy reform to ensure equitable medication pathways for all.
Read the full report here.


 ROS and APPG on Osteoporosis and Bone Health Inquiry Report on Access to Medicines
ROS and APPG on Osteoporosis and Bone Health Inquiry Report on Access to Medicines

 The All Party Parliamentary Group (APPG) for Osteoporosis and Bone Health published a report into the long-standing postcode lottery in the NHS for osteoporosis care. The report highlights the scale of under-diagnosis, under-treatment and missed opportunities in the NHS, with a blueprint for change. Implementation of the blueprint in England and Wales could save the NHS around £287m over five years – a return on investment of around 3:1 – according to the Royal Osteoporosis Society (ROS), which has supported the Inquiry.…
The All Party Parliamentary Group (APPG) for Osteoporosis and Bone Health published a report into the long-standing postcode lottery in the NHS for osteoporosis care. The report highlights the scale of under-diagnosis, under-treatment and missed opportunities in the NHS, with a blueprint for change. Implementation of the blueprint in England and Wales could save the NHS around £287m over five years – a return on investment of around 3:1 – according to the Royal Osteoporosis Society (ROS), which has supported the Inquiry.… 

 by Ellie Davies, Acting Project Manager, Falls and Fragility Fracture Audit Programme (FFFAP)
by Ellie Davies, Acting Project Manager, Falls and Fragility Fracture Audit Programme (FFFAP)
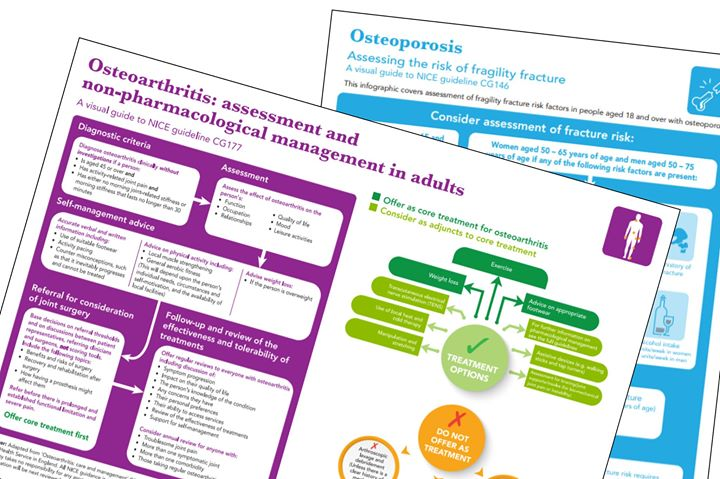

 On 30th November 2017, the National Osteoporosis Society published new Osteoporosis Standards and Vertebral Fractures Guidance for Health Professionals. The guidelines help health professionals provide the possible care for people with osteoporosis.
On 30th November 2017, the National Osteoporosis Society published new Osteoporosis Standards and Vertebral Fractures Guidance for Health Professionals. The guidelines help health professionals provide the possible care for people with osteoporosis.
 Read the
Read the